
About the Department of Anesthesiology and Perioperative Medicine
Residency
Anesthesiology Residency Program
The mission of the Anesthesiology Residency Program is to cultivate, train, and mentor our anesthesiology residents to achieve success in both their professional and personal lives. Residents are exposed to diverse cases and graduate from the program with a tremendous clinical experience that we feel truly prepares them to be expert consultants in anesthesiology.
Fellowships
Accordion Content
-
We offer an ACGME accredited 1-year fellowship in Adult Cardiothoracic Anesthesia. The goal of the fellowship is to provide an academic environment and enough clinical substrate to ensure that the fellow achieves a level of autonomy in delivering anesthetic care for complex cardiac surgery.
Discover More About the Adult Cardiothoracic Anesthesia Fellowship
-
Our interventional pain medicine fellowship is an ACGME-accredited 1 year program dedicated to advanced training in the management of acute, chronic, and oncology-related painful conditions presenting in a busy metropolitan hospital. We offer a diverse range of services and provide Pain Management Specialty training with weekly didactic activities which greatly enhances the knowledge and expertise of our pain specialists.
Discover More About the Interventional Pain Medicine Fellowship
Clerkship
The Department of Anesthesiology and Perioperative Medicine offers an elective in perioperative care to all medical/dental students.
The main purpose of our clerkship program is to allow students to become familiar with the field of anesthesia and what it entails to safely manage a patient through their perioperative period. The goals of the clerkship elective:
- To give medical/dental residents/students an appreciation of the anesthesia field.
- To teach techniques of preoperative evaluation. To recognize those patients and situations that pose an increased anesthetic risk, and to optimize preoperative therapy for such patients to minimize this risk.
- To teach the characteristics of commonly used anesthetic agents and techniques and their risks and complications.
- To acquaint medical students with the principles and skills involved in airway management, intraoperative fluid therapy and the proper use of intraoperative monitors
While the clinical practice of anesthesia has had a long and interesting history, it is only in the last 50 years that the specialty of anesthesiology has become a fully recognized medical discipline. It now requires of its practitioners a broad working knowledge of pharmacology, physiology, pulmonary medicine, cardiology, endocrinology, surgery, obstetrics, pediatrics and electronics. In addition, the anesthesiologist must be skilled in airway maintenance, regional techniques and invasive monitoring. Other than the management of the patient in the perioperative period, this specialty is strongly committed to:
- Teaching cardiopulmonary resuscitation
- Critical care medicine
- The treatment of acute and chronic pain
- Research
Student Information
Students can call the Anesthesia Clinical Office at (732) 937-8841 and ask for Dr. Alexander Kahan or Dr. Christopher Fjotland. Students will meet with Dr. Zuker/Fjotland in the anesthesia clinical office located on the 1st floor of Robert Wood Johnson University Hospital (across from the Medical Records Department) at 7:00 a.m. sharp for their first assignment. Students are asked to read over our handout before they report for their anesthesia rotation.
Contact Information
Students may contact Dr. Dora Zuker by e-mail or Dr. Christopher Fjotland by email.
Human Patient Simulator (HPS)
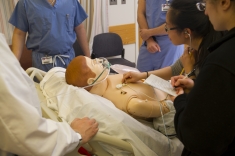
The department operates one adult, "NORMAN" (NORmal MAN), and one baby computerized human patient simulator (HPS) that provide educational opportunities for medical students, anesthesia residents, and even more experienced attending anesthesiologists.
Our HPS, the only one in New Jersey, is a three-dimensional interactive model.
It combines lifelike hardware with computerized physiologic models of human organ systems. Physically, the simulator looks and sounds like a real patient. It has a head with blinking eyelids, reactive pupils and a controllable airway. The pulses are palpable, the breath and heart sounds are audible, it breathes and has an arm that twitches with stimulation. The simulator is monitored like any patient in the operating room complete with ECG, pulse oximetry, mean arterial, pulmonary artery and central venous pressure tracings. Computer models run these systems, accurately emulating human physiology. Parameters can be set to control how each system functions and responds to interventions. The simulator employs a pharmacologic system that produces realistic dose-related pharmacokinetic and pharmacodynamic responses to injected or inhaled "drugs."
The result is an interactive model that can be "anesthetized" and managed through a variety of scenarios that provide educational opportunities for medical students, anesthesia residents and even more experienced attending anesthesiologists.
Healthcare providers interested in learning further about the Robert Wood Johnson simulator may contact Mordechai Bermann, MD, Director of the Human Patient Simulator Lab, by phone (732) 235-6153 or by email.
Life at Rutgers

Envision Yourself Here
Rutgers is located in central New Jersey in the city of New Brunswick and across the Raritan River in Piscataway. Middlesex-Somerset-Hunterdon counties rank fourth in per capita income nationwide. It is a manufacturing center, agricultural center, high-tech corporate center, and small-town America rolled into one.
Who We Are
Explore the list of accomplished faculty comprising the Department of Anesthesiology and Perioperative Medicine.
Faculty by Subspecialty
Our faculty teach in a variety of subspecialty areas related to the field of anesthesiology.
Accordion Content
-
Keith P. Lewis, RPh, MD
Chair Anesthesiology Department
Phone: 732-235-7246
Fax: 732-418-8492Antonio Chiricolo, MD
Associate Professor
Exec Vice Chair, Clinical Affairs
Phone: 732-235-7246
Email: chirican@rwjms.rutgers.edu
Fax: 732-418-8492Sagar Mungekar, MD
Assistant Professor
Vice Chair, Information Systems and Analytics
Phone: 732-235-7246
Email: sagarms@rwjms.rutgers.edu
Fax: 732-235-6131 -
Enrique Pantin, MD
Professor
Division Chief Cardiothoracic Anesthesiology
Chief, Section of Intraoperative Ultrasound
Phone: 732-235-7246
pantinej@rwjms.rutgers.eduAntonio Chiricolo, MD
Associate Professor
Vice Chair, Clinical Affairs
Chief, Section of Thoracic Anesthesia
Phone: 732-235-7246
chirican@rwjms.rutgers.eduSagar Mungekar, MD
Associate Professor
Vice Chair, Information Systems and Analytics
Phone: 732-235-7246
sagarms@rwjms.rutgers.edu
Brian Raffel, MD
Associate Professor
Program Director, Cardiothoracic Fellowship
Phone: 732-235-7246
brian.raffel@rwjms.rutgers.eduVincent Reformato, MD
Assistant Professor
Chief, Section of Vascular Anesthesia
Phone: 732-235-7246
vr247@rwjms.rutgers.eduJulie Wise, MD
Assistant Professor
Phone: 732-235-7246
wiseja@rwjms.rutgers.eduEileen Kodack, MD
Associate Professor
732-235-7246
ek799@rwjms.rutgers.eduAsim Raja, MD
Associate Professor
Phone: 732-235-7246
ar2263@rwjms.rutgers.eduTeuta Marsic, MD
Assistant Professor
Phone: 732-235-7246
tm1024@rwjms,rutgers.eduPooja Patel, MD
Assistant Professor
Phone: 732-235-7246
pkp52@rwjms.rutgers.eduDenes Papp, MD (semi-retired)
Professor of Anesthesiology
Phone: 732-235-7246
pappde@rwjms.rutgers.eduMaciej Nawracaj, CRNA
Clinical Coordinator SRNA Program
Phone: 732-235-7246
nawracm1@rwjms.rutgers.eduVivian Gao, CRNA
Phone: 732-235-7246
vyg1@rwjms.rutgers.eduChrista VIllaluna, CRNA
Phone: 732-235-7246
risluna@rwjms.rutgers.edu -
Christine Fratzola, MD
Chief Professor
Phone: 732-235-7246
Email: Christine.Hunter@rutgers.edu
Fax: 732-418-8492Sylviana Barsoum, MD
Professor
Phone: 732-235-7246
Email: barsous@rwjms.rutgers.edu
Fax: 732-418-8492Asim N. Raja, MD
Associate Professor
Phone: 732-235-7246
Email: asim.raja@rwjms.rutgers.edu
Fax: 732-418-8492Janak Bhatt, MD
Clinical Instructor
Phone: 732-235-7246
Email: jb1668@rwjms.rutgers.edu
Fax: 732-418-8492Shaul Cohen, MD
Professor
Phone: 732-235-7246
Fax: 732-418-8492Jennifer Cowell, MD
Assistant Professor
Phone: 732-235-7246
Fax: 732-418-8492Christopher W. Fjotland, MD
Assistant Professor
Phone: 732-235-7246
Email: christopher.fjotland@rutgers.edu
Fax: 732-418-8492Geza Kiss, MD
Professor
Phone: 732-235-7246
Email: kissgk@rwjms.rutgers.edu
Fax: 732-418-8492Benjamin Landgraf, MD
Adjunct Assistant Professor
Phone: 732-235-7246
Email: landgrbr@rwjms.rutgers.edu
Fax: 732-418-8492Edward Mosenkis, MD
Clinical Instructor
Phone: 732-235-7246
Email: em1052@rwjms.rutgers.edu
Fax: 732-235-6131Geraldo Rodriguez, MD
Associate Professor
Phone: 732-937-8841
Email: gr462@rwjms.rutgers.edu
Fax: 732-418-8492Mina Morgan, MD
Assistant Professor
Phone: 732-235-7246
Email: morganm3@rwjms.rutgers.edu
Fax: 732-418-8492James T. Tse, MD
Professor Clinical Track Scholar
Phone: 732-235-7246
Email: tsejt@rwjms.rutgers.edu
Fax: 732-418-8492 -
William Grubb, MD
Chief Associate Professor
Phone: 732-235-7246
Email: grubbwr@rwjms.rutgers.edu
Fax: 732-418-8492Robert Jongco, MD
Assistant Professor
Phone:732-235-7246
Email: jongcoro@rwjms.rutgers.edu
Fax: 732-418-8492Mina Gaballa, MD
Assistant Professor
Phone:732-235-7246
Email: mgaballa@rwjms.rutgers.edu
Fax: 732-418-8492Alopi Patel, MD
Associate Professor
Phone:732-235-7246
Email: patel154@rwjms.rutgers.edu
Fax: 732-418-8492 -
Valerie McRae, MD
Chief, Division Pediatric Anesthesia
Associate Professor
Phone: 732-235-7246
Email: mcraeva@rwjms.rutgers.edu
Fax: 732-418-8492Aaron Bernotas, MD
Assistant Professor
Phone: 732-235-7246
Email: ab1888@rutgers.edu
Fax: 732-418-8492Ryan Fields, MD
Assistant Professor
Phone: 732-235-7246
Email: rf547@rwjms.rutgers.edu
Fax: 732-418-8492Samuel Y. Kiel, MD
Assistant Professor
Phone: 732-235-7246
Email: kielsy@rwjms.rutgers.edu
Fax: 732-418-8492Alvin Kim, MD
Assistant Professor
Phone: 732-235-7246
Email: ak2036@rwjms.rutgers.edu
Fax: 732-418-8492Temitope Okuwa, MD
Assistant Professor
Phone: 732-235-7246
Fax: 732-418-8492Enrique Pantin, MD
Professor
Phone: 732-235-7246
Email: pantinej@rwjms.rutgers.eduJessica Perez Mahajan, MD
Assistant Professor
Phone: 732-235-7246
Email: j.perez.md@rutgers.edu
Fax: 732-418-8492Usman Shah, MD
Associate Professor
Phone: 732-235-7246
Email: us77@rwjms.rutgers.edu
Fax: 732-418-8492Dora Zuker, MD Associate Professor
Phone: 732-235-7246
Email: zukerdd@rwjms.rutgers.edu
Fax: 732-418-8492
Certified Registered Nurse Anesthetist (CRNA)
Accordion Content
CRNA stands for Certified Registered Nurse Anesthetist. We are a highly skilled group of advanced practice nurses with masters and/or Doctorate degrees. We work in a care team model with our attending anesthesiologist colleagues. We provide anesthetics for a wide variety of cases including cardiac, pediatrics and obstetrics. We work together in a professional, collegial environment that is both challenging and exciting.
-
- Stacey Paulus, CRNA/APN, Assistant Professor Prof Prac, Chief CRNA
- Temitope Ajibade
- Susan Bauer
- Bruno Beja-Umukoro
- Brian Gaeta
- Vivan Gao
- Rachel Landgraf
- Terence McBride
- Mariah McGrory
- Mamdoh Michael
- Aleksandr Myachikov
- Maciej "Matt" Nawracaj
- Zlata Polyaeva
- Vanessa Rodriguez
- Elzbieta (Liz) Samojluk
- Maria Tobias
- Kim Trojak
- Nancy Tuano
- Christa Joy Villaluna
- Donglei Yan
- Haseya Abdoul-Karim
- Folasade Ajisegbede
- Maria del Carmen Fleites
- James Doran
- Kristine Doris
- Tatiana Figueroa
- Lucy Foster
- Catherine Gerace
- Jessica Grevesen
- Claire Latourette
- David McNally
- Patrick O'Dunne
- Angeli Grace Parham
- Timothy Shi
- Hosana Tordecilla
- Susan Welsh
- Tom Zimmerman
- Jacqueline Carrozza
- Hannah Mandler
- Dayane Richards
- Jenna Bloss
-
- Hosana Tordecilla
- Claire Latourette
- Jessica Grevenson
- Alison Groden
- Bernadette Antunes
- Folasade Ajisegbede
- Alexandra Rozhitsky
- Andres Sepulveda
- Catherine Gerace Quigley
- Tatiana Figueroa
- Tom Zimmerman
- Susan Welsh
- Elzbieta Samojluk
- Nancy Tuano
- Zlata Polyaeva
- Neda Blagojevik
- Maria del Carmen Fleites
- James Doran
- Kristine Doris
- Lucy Foster
- Maksim Ivanouski
- Terence McBride
- Patrick O'Dunne
- Angeli Grace Parham
- John Yoo
About
The Department of Anesthesiology and Perioperative Medicine at the Robert Wood Johnson Medical School trains and mentors medical students, residents, and fellows in the fields of anesthesiology and pain management. We offer two anesthesia electives for fourth-year medical students, and a complete anesthesiology residency program as well as fellowships in cardiothoracic anesthesiology and interventional pain medicine.
Meet the Chair

Keith P. Lewis, RPh, MD, Professor and Chair, Department of Anesthesiology and Perioperative Medicine—who began his career in pharmacy and cancer chemotherapy at Yale University—brings focus and motivation to improving periprocedural safety and rethinking processes. “I pursued a career in pharmacy first. I was always intrigued about the safety element of medicine,” he says. “When I worked in a cancer chemotherapy clinic, the person who hired me told me I would be a good candidate for medical school—and here I am.” Dr. Lewis’ résumé is a testament to his never-ending pursuit of changing the paradigm.
At Boston University School of Medicine and Boston Medical Center (BMC), Dr. Lewis served as professor and chair, Department of Anesthesiology, and chief of anesthesiology, respectively. He facilitated the merging of the Boston City Hospital and Boston University Medical Center Hospital operating rooms. He served for 20 years as a senior anesthesiologist and is a past president of Anaesthesia Associates of Massachusetts—one of the largest academic and private practices in the Boston area. There, he helped to develop a high-risk bariatric surgery program, a state-of-the-art multimedia center, a multidisciplinary pain clinic, and a surgical robotics program, among others. He also helped to establish a cutting-edge simulation center focusing on team training. Under his leadership, his department received multiple nationally recognized safety awards.
Practicing anesthesiology led to Dr. Lewis’ development of imaginative workspace designs. He gained renown for the conceptualization and design of the Moakley Ambulatory Surgery Center’s “ORs of the Future” at BMC—six ambulatory operating rooms with fast-track anesthesia techniques. Last fall, BMC introduced the Integrated Procedural Platform, another concept that Dr. Lewis helped to design, which consolidates all procedural-based specialties side by side on one floor, facilitating integrated care for patients requiring interventional procedures.
Dr. Lewis’ educational background speaks to his inner drive for constant discovery. He completed his internship in surgery at New England Deaconess Hospital and his anesthesiology residency training at Brigham and Women’s Hospital after receiving his medical degree from the University of Connecticut School of Medicine. Dr. Lewis also trained in cardiac anesthesia at Brigham and Women’s Hospital and served on the Harvard faculty for 14 years prior to joining Boston University School of Medicine.
The general theme throughout Dr. Lewis’ career has been to minimize or eliminate the variables that can impact patient safety. He designed and rolled out the official universal Protocol focusing on quality and patient safety at BMC, and he has received national awards for that and other safety initiatives. Not only did he spearhead a national symposium, “Positioning Your ORs for the Future,” but, with his team, he wrote a book on patient safety, OK to Proceed? What Every Healthcare Provider Should Know about Patient Safety. “The book’s 52 chapters offer strategies on how to potentially avoid adverse outcomes,” Dr. Lewis says. “It’s all about making the experience the safest for our patients.”
In addition to chairing the Department of Anesthesiology and Perioperative Medicine at Robert Wood Johnson Medical School, Dr. Lewis is serving as chief of anesthesia and director of perioperative quality and safety at Robert Wood Johnson University Hospital, an RWJBarnabas Health facility. He sees enormous potential for synergy. “I am excited that there is so much passion and commitment here, and that everyone is invested in the concept of patient safety and streamlining and improving the way we practice,” he says. “I feel like this is an outstanding opportunity to create leading-edge changes, providing the best value-based integrated care and putting the patient at the center of it all.”
Along with changing traditional practice and revolutionizing processes, Dr. Lewis also looks forward to what he calls “flipping the classroom” by integrating simulation into the educational experience. He sees great value in utilizing new technological advances to train all health care staff.
The holistic goal, as always, is to work with the community to make it healthier. That requires a willingness to look at things differently. He believes there is great benefit in seeing things from many perspectives while making active listening central to his management style. One thing is for certain: he can’t wait to see where all of this new energy leads.
Administration
Amy Smith
Sr. Director of Administration
Department of Anesthesiology and Perioperative Medicine
Department of Emergency Medicine
as2568@rwjms.rutgers.edu
Judy Keller
Executive Assistant to Dr. Keith P. Lewis, Professor and Chair
Vice Dean, Robert Wood Johnson Medical School
Department of Anesthesiology and Perioperative Medicine
judy.keller@rutgers.edu
Allyn Brillant
Quality Coordinator
Department of Anesthesiology and Perioperative Medicine
ab2271@rwjms.rutgers.edu
Doreen M. Stillwell
Residency/Fellowship Program Supervisor
Department of Anesthesiology and Perioperative Medicine
stillwdm@rwjms.rutgers.edu
Martha Caldera
Residency Program Assistant
Department of Anesthesiology and Perioperative Medicine
caldermv@rwjms.rutgers.edu
Kathy Idrissi
Program Coordinator to Sr. Director of Administration Amy Smith
Department of Anesthesiology and Perioperative Medicine
kmi22@rwjms.rutgers.edu
Jessica Waters
Program Assistant
Department of Anesthesiology and Perioperative Medicine
jw1635@rwjms.rutgers.edu
Danielle Plyler
Billing & Coding Analyst
Department of Anesthesiology and Perioperative Medicine
plylerde@rwjms.rutgers.edu
Anupreet Singh
Billing & Coding Analyst
Department of Anesthesiology and Perioperative Medicine
as3737@rwjms.rutgers.edu
Division of Cardiothoracic Anesthesiology
Cardiac care has been one of the cornerstones of the clinical arena since the early days at Robert Wood Johnson University Hospital. Our division has a long history of pursuing new techniques in the management of patients requiring anesthetic care, enabling them to return to their previous state of health and back to everyday life. In the 90’s our hospital was an early adopter of biventricular support with the Abiomed BVS-5000, and the Heartmate I as bridge to transplant. Since those days we have continued to adapt to newer ventricular support as technology evolves. Techniques such as minimally invasive cardiac surgery (MICS) were started at our center in 2004 and with that, we modified our practice to match the evolution seen in cardiac surgery. Fast-track cardiac anesthesia and enhanced recovery were a natural progression from the MICS concept. This has been championed by our team since at least 2009 with a number of goals set to improve outcomes and the patient experience without increasing the rate of adverse events. These goals include extubating within 2 hours of admission to the ICU, discharge from the ICU within 24 hours, and discharge from the hospital within 5 days. These were radical concepts in those days. We did have a short window into pediatric cardiac surgery in 2005 when our hospital created a Pediatric Cardiac Surgery Program with Columbia University as its partner. The only two services at RWJUH that were able to tackle care for these patients independently of the Columbia affiliation were the Perfusion Services and our Division. Other milestones achieved at our center include the first insertion after FDA clearance of the totally implantable artificial heart, the AbioCor, in 2009. With the advent of transcatheter technologies, we were early adopters, our experience continues to grow with different clips, aortic, mitral, and tricuspid alternatives being made available.
Another leap forward that we took a few years ago was the adoption of preoperative erector spinae blocks for all our cardiac surgery patients allowing for the use of minimal or, in some cases, no intraoperative opioids. With this approach, we now extubate more than 50% of all our cardiac surgery cases in the operating room. The continued evolution in cardiothoracic care will continue to favor our proactive and adaptative view of the future!
Teamwork is the hallmark of our division. We have a close-knit group of cardiothoracic anesthesiologists who are always happy to work together and lend a hand. We often collaborate on complex cases and there is no shortage of support when needed. Senior faculty members provide excellent support and mentorship for the junior faculty, helping to grow their skills and knowledge set as well as find opportunities for career development.
We are a team that loves what they do and strives to be progressive, always looking forward!
Visit us here for information related about our Cardiothoracic Anesthesia Fellowship and our Cardiothoracic Anesthesia Faculty
Accordion Content
-
06-10-07 TEE Pericardial Effusion
03-14-08 Aortic Valve short axis view
03-16-08 Transesophageal Echocardiography LVH
03-16-08 Lighted Wand / Estilete Luminoso
01-31-09 Airway Pediatric 3m 070308 2
01-31-09 Airway Pediatric 3m 070308 2
01-31-09 Pediatric airway 070208 3y
02-03-09 TECNICAS DE AISLAMIENTO PULMONAR PARTE 1
02-03-09 TECNICAS DE AISLAMIENTO PULMONAR Parte 2
05-28-11 Minimally Invasive Cardiac Surgery central line insertion
11-13-11 Lung isolation techniques
10-31-14 Descending thoracic aorta atheroma
10-16-14 3D Normal Aortic and Mitral valve
10-21-14 TEE Bicuspid aortic valve with stenosis and insufficiency
10-31-14 Válvula Aortica y Mitral normales en 3D y eco Doppler
10-31-14 normal Aortic and Mitral Valves with CFD
04-13-15 Bioprosthetic mitral valve with large paravalvular leaks
10-30-15 Hypotension post cardiac catheterization
2-21-2015 The Transplant Experience: From the Professional and Personal Perspective
07-14-16 Válvula Aórtica Bicúspide
07-14-16 Bicuspid Aortic Valve
09-25-16 Incidental Finding of a Ventricular Septal Defect
09-25-16 Hallazgo Intraoperatorio Incidental de Defecto Interventricular
06-12-17 Mixoma Cardiaco – Tumor Cardiaco
06-12-17 Cardiac Myxoma – Cardiac Tumor
10-25-17 Mitral Valve endocarditis and Coronary Artery Disease
10-25-17 Vegetación valvular mitral en 2D y 3D
11-05-17 Coronary sinus anatomy by TEE
11-05-17 Ecocardiografía transesofágico (ETE) del Seno Coronario en 2D y 3D
03-18-18 Electrodo de Marcapasos Cardiaco Transvenoso Perforando el Ápex del Ventrículo Derecho
03-18-18 Pacemaker-Defibrillator Pacer Lead Perforating the Right Ventricle
05-15-19 Mitral Stenosis Rheumatic Heart Disease: Apical View 4 chamber
05-15-19 Mitral Stenosis Rheumatic Heart Disease: ParaSternal Long mitral valve Color Flow Doppler
05-15-19 Mitral Stenosis Rheumatic Heart Disease: ParaSternal Long mitral valve
05-15-19 Mitral Stenosis Rheumatic Heart Disease: ParaSternal Short Mid View of the LV and RV
03-28-20 Using an anesthesia machine as an ICU ventilator: Drager Apollo basic concepts
03-28-20 Using an anesthesia machine as an ICU ventilator: GE Avance basic concepts
04-04-20 3 types of high level airway protection PPE made with hospital standard supplies
04-21-20 Intra-aortic balloon pump (IABP) inflated seen in Computed Tomography (CT)
04-25-20 Stab wound to the heart
05-08-20 Chest Computed Tomography (CT) with pleural and pericardial effusions
05-15-20 Right Internal Jugular Vein Obstruction Diagnosed During Heart Surgery
11-15-20 Aortic cusp fold causing Aortic Insufficiency
11-25-2 1 Técnicas de acceso vascular ecoguiado (CASTELLANO / SPANISH)
01-01-22 Tracheal origin of right upper lobe. Right tracheal bronchus ("pig bronchus").
01-27-22 Vascular access with ultrasound
03-27-22 Severe Bioprosthetic Transvalvular Regurgitation Post Mitral Valve Replacement
Accordion Content
-
Enrique Pantin, MD
Professor of Anesthesiology and Perioperative Medicine
Division Chief, Cardiothoracic Anesthesiology
pantinej@rwjms.rutgers.eduDenes Papp, MD
Professor of Anesthesiology and Perioperative Medicine
pappde@rwjms.rutgers.eduAntonio Chiricolo, MD
Associate Professor of Anesthesiology and Perioperative Medicine
Vice Chairman, Clinical Affairs, Chief, Section Thoracic Anesthesia
chirican@rwjms.rutgers.eduBrian Raffel, DO
Assistant Professor of Anesthesiology and Perioperative Medicine
Fellowship Program Director
brian.raffel@rutgers.eduSagar Mungekar, MD
Assistant Professor of Anesthesiology and Perioperative Medicine
Vice Chair, Information Systems & Analytics
sagarms@rwjms.rutgers.eduVincent Reformato, MD
Assistant Professor of Anesthesiology and Perioperative Medicine
vr247@rwjms.rutgers.eduJulie Wise, MD
Assistant Professor of Anesthesiology and Perioperative Medicine
wiseja@rwjms.rutgers.eduAsim N. Raja, MD
Associate Professor of Anesthesiology and Perioperative Medicine
asim.raja@rwjms.rutgers.eduEileen Kodack, DO
Assistant Professor of Anesthesiology and Perioperative Medicine
ek799@rwjms.rutgers.eduTeuta Marsic, MD
Assistant Professor of Anesthesiology and Perioperative Medicine, and Critical Care
tm1024@rwjms.rutgers.eduPooja Patel, MD
Assistant Professor of Anesthesiology and Perioperative Medicine
pkp52@rwjms.rutgers.eduMaciej Nawracaj, CRNA
nawracm1@rwjms.rutgers.eduVivian Gao, CRNA
vyg1@rwjms.rutgers.eduPhone: 732-937-8841, 732-235-7246
Fax: 732-418-8492
Accordion Content
-
Dr. Alann Solina 1995 --- February 29, 2016
--First Section Head of Cardiac Anesthesiology:1995-2001
--First Division Head of Cardiac Anesthesiology: 2001-2015
Dr. Denes Papp --- March 1, 2016-June 30, 2022
Dr. Enrique J. Pantin --- July 1, 2022 -
Research Activities
Faculty, fellows, residents, and students have a great opportunity to engage in academic and scholarly activities at Robert Wood Johnson Medical School’s Department of Anesthesiology and Perioperative Medicine. We consider participation in scholarly activities to be an essential component of education and faculty development.
The major focus of our research laboratory has been to investigate, how the integrity of the blood- brain barrier(BBB) and cerebral microregional oxygen balance could be altered by anesthetics in various pathological conditions. In addition, intracellular signaling, neurotransmitters, and various factors and receptors have been investigated in focal cerebral ischemia. Recently, we are studying microregional oxygen balance in an animal model of tuberous sclerosis-autism spectrum disorders and the role of mTOR related pathways in BBB disruption during early cerebral ischemia-reperfusion.
Publications and Abstracts
Accordion Content
-
Recent Publications
(Students, Residents, Fellows are bolded)
Textbooks:
- Anesthesia Unplugged, McGraw Hill, 2012, Edited by Steven H. Ginsberg MD and Chris Gallagher MD.
- TEE: Board Stiff, McGraw Hill, accepted for publication 2012. Edited by Steven H. Ginsberg MD and Chris Gallagher MD.
Book Chapters:
- Anesthesia Unplugged, Ginsberg S MD & Gallagher C MD, McGraw Hill, 2012.
- Solina, Zhou: Internal Jugular Access
- Kertsman, DeAngelis: Femoral Venous Access
- Barsoum: Femoral Arterial Access
- LaSalle, Kiss, Denny: Awake Intubation
- Daley, Denny, Batsides: Emergency Airway
- Kraidin, DeLara, Langenfeld: Thoracic Epidurals
- Hall, Panjwani: Blood Patch
- Kiss, Kuppasamy, Lasalle: Regional BLock of the Upper Extremity
- McDonough, Saluja, Kraidin, A Khan: Pacing
- K Khan, Pantin: TEE
- Wong, Chhokra: Smooth Emergence
- Mehta, Hunter: Positioning
- Grubb, Chaung D: Cath Lab Anesthesia
- Janco, Kaufman, Ginsberg, Kraidin: Handoff for PACU and ICU
- Kraidin, Anderson, Ginsberg: Port Access
- Slomovits, Ginsberg: PAT
TEE: Board Stiff, McGraw Hill, accepted for publication 2012. Edited by Steven H. Ginsberg MD and Chris Gallagher MD.
- Ginsberg, Kraidin: Equipment, Infection, and Safety
- Kraidin, Ginsberg, Jian: Principles of Doppler Ultrasound
- Aldo, Pantin: Pathology of the Cardiac Valves
- Pantin, Aldo: Pericardium and Extra-Cardiac Structures
- Solina, Aldo, Zisa: Cardiac Masses
- Grubb, Burr: Test Questions
Kaplan’s Cardiac Anesthesia, Sixth Edition, Edited by Kaplan, Reich, and Savino, W.B. Saunders, 2011.
- Augoustides J, Pantin E, Cheung A: The Echo Era
Manuscripts:
- Kraidin J, Ginsberg S, Pantin E, Veksler B, Anderson M, Fisch D, and Solina A: Left Atrial Mass During a Minimally Invasive Thoracic Mitral Valve Replacement. J. Cardiothoracic and Vascular Anesthesia, Vol 25, No 2, p376-7, 2011.
- Kraidin, Jonathan L. MD; Pantin, Enrique J. MD; Anderson, Mark B. MD; Zhou, Bo-Lu MD; Solina, A MD: Edwards EndoVent as a Pacing Catheter for Minimally Invasive Aortic Valve Surgery: A Novel Approach, Innovations: Technology & Techniques in Cardiothoracic & Vascular Surgery. Volume 6 - Issue 4 - pp 253-256, August, 2011.
- Kraidin J, Ginsberg S, Solina A: "Anesthesia Apps: Overview of current technology and intelligent search techniques". Journal of Cardiothoracic and Vascular Anesthesia, Volume 26, Issue 2, Pages 322-326, April 2012.
- Pantin E, MD, Kraidin J, MD, Ginsberg S, MD, Denny J, MD, and Solina A, MD: Cannulation of the Middle Cardiac Vein during MICS, Innovations: Technology and Techniques in Cardiothoracic and Vascular Surgery, Vol 7.Pantin E, Kraidin J, Ginsberg S, Denny J, Anderson M, Solina A: The Swan-Ganz Catheter as a Teaching Tool for the Anesthesiologist Learning Minimally Invasive Cardiac Surgery, accepted for publication in Technology and Techniques in Cardiothoracic and Vascular Surgery, 7(3), p204-207, 2012.
- Pantin E, Kraidin J, Ginsberg S, Denny J, Anderson M, Solina A: The Swan-Ganz Catheter as a Teaching Tool for the Anesthesiologist Learning Minimally Invasive Cardiac Surgery, accepted for publication in Technology and Techniques in Cardiothoracic and Vascular Surgery, 7(3), p204-207, 2012.
- Ginsberg S, Kraidin J, Grubb W, Panjwani S, Solina A: Noise in the Operating Room during Cardiac Surgery. Accepted for publication, J. Cardiothoracic and Vascular Anesthesia, No. JCVA-D-12-00308R1, 2012.
- Oak Z.Chi, MD, Christine Hunter, MD, Xia Liu, MD, Youngchan Chi, Harvey R. Weiss: Effects of GABAA receptor blockade on regional cerebral blood flow and blood-brain barrier disruption in focal cerebral ischemia. Journal of the Neurological Sciences; 301 (2011) 66-70.
- Oak Z Chi, MD, Christine Hunter, MD, Xia Liu, MD, and Harvey R. Weiss, PhD: The Effects of Dexmedetomidine on Regional Cerebral Blood Flow and O2 Consumption during Severe Hemorrhagic Hypotension in Rats. Anesthesia & Analgesis, 2011; 113 (2): 349-55.
- Oak Z, Chi, Jeremy Grayson, Sylviana Barsoum, Christine Hunter, Xia Liu, Harvey R. Weiss. Effects of a PDGFR-a Antagonist Imatinib on Blood-Brain Barrier Disruption in Focal Cerebral Ischemia in Younger and Older Rats. J Neurol Res; 2012: 2(4): 127-133.
-
Abstracts and Poster Presentations:
- Amponsah A, Ginsberg S, Kraidin J, Solina A: Equipment Availability and Patient Safety Survey, Presented at Annual NJSSA Meeting, April, 2011.
- Amponsah A, Ginsberg S, Kraidin J, Solina A: Equipment Availability and Patient Safety Survey, Presented at Annual IARS Meeting, May, 2011.
- Ginsberg S MD, Kraidin J MD, Aldo L MD, Gallagher C MD, Hoover D PhD MPH, and Solina A MD: “Inadequate Anesthesia Technician and Transport Support at Academic Anesthesia Departments in the United States”. Post Graduate Assembly of the New York State Society of Anesthesiologists, 2011.
- S Ginsberg MD, J Kraidin MD, K Khan MD, C Gallagher MD,D Hoover PhD MPH, and A Solina MD: “Inadequate Professional Staffing of AcademicAnesthesia Departments in the United States”, PGA of NYSSA, 2011.
- James Tse, Maria Negron-Gonzalez, Batul Razvi, John Denny, Scott Mellender and Shaul Cohen: Pre-Oxygenation with No-Cost TSE “Mask” Reduces Severe Desaturation and Improves Oxygenation in Obese Patients under Deep Propofol Sedation during Lengthy Upper GI Endoscopy. Poster Presentation (S-157) at the IARS 2011 Annual Meeting, Vancouver, British Columbia , Canada, May 21-24, 2011.
- J Tse, M Negron-Gonzalez, B Razvi, J Denny, S Mellender and S Cohen: Pre-Oxygenation with No-Cost TSE “Mask” Reduces Severe Desaturation and Improves Oxygenation in Obese Patients under Deep Propofol Sedation during Lengthy Upper GI Endoscopy. Poster Presentation (S-157) at the IARS 2011 Annual Meeting, Vancouver, British Columbia , Canada, May 21-24, 2011.
- S Barsoum, S Cohen, J Denny, D Chyu, P Patel, M Kaufman, S Yeh, A Kahan and J Tse: Pre-Oxygenation with No-Cost TSE “Mask” Reduces Severe Desaturation in Patients under Deep Propofol Sedation during Short Upper GI Endoscopy. Poster Presentation (P9018) at the NYSSA 65th PostGraduate Assembly in Anesthesiology, NY, Dec 9-13, 2011.
- K Dauphinee, H Razo, M Y. Khan, S Cohen, S Barsoum, A Mohiuddin and J Tse: Does Pre-Oxygenation with a No-Cost TSE “Mask” Reduce Severe Desaturation in Elderly Patients under Deep Propofol Sedation during Upper GI Endoscopy? Poster Presentation at the SAMBA 27th Annual Meeting, Miami, FL, May 3-6, 2012.
- J Tse, B Collins, K Dauphinee, T Mehta, C Hunter, L Spina and S Cohen: Pre-Oxygenation with a No-Cost TSE “Mask” Prevents Severe Desaturation and Reduces the Need for Bag-Mask Ventilation in Elderly Patients under Deep Propofol Sedation during Upper GI Endoscopy. Poster Presentation (S284) at the IARS 2012 Annual Meeting, Boston, MA, May 18-21, 2012.
- M Bermann, S Cohen, M Khan and J Tse: Pre-Oxygenation with No-Cost TSE "Mask" Prevents Severe Desaturation and Improves Oxtgenation in Obese Patients under Deep Propofol Sedation during Lengthy Upper GI Endoscopy. Poster Presentation (#61) at the 2012 Meridian Health Research Day, NJ June 12, 2012.
- J Tse, S Cohen, Br Collins, J Denny, S Barsoum, L Spina, K Dauphinee, M Fernandez, M Wu, C Hunter: Is No-Cost TSE “Mask” More Efficient than High Nasal Cannula Oxygen Flow in Reducing Severe Desaturation in Patients under Deep Propofol Sedation during Upper GI Endoscopy? Poster Presentation (A768) at the 2012 ASA Annual Meeting, Washington, D.C., Oct 13-17, 2012.
- M Negron-Gonzalez, D Zuker, S Cohen, J Denny, J Mathew and J Tse: A Simple Technique to Reduce Severe Desaturation in Propofol-Sedated Patients during Short Upper GI Endoscopy. Poster Presentation (394) at the 15th WFSA World Congress of Anaesthesiologists, Buenos Aires, Argentina, March 25-30, 2012
- Sylviana Barsoum, Shaul Cohen, Maria Negron-Gonzalez, Sumita Bery, Christine W. Hunter and James Tse: No-Cost TSE “Mask” Prevents Severe Desaturation in Elderly Patients under Deep Propofol Sedation during Upper GI Endoscopy. Poster Presentation (876) at the 15th WFSA World Congress of Anaesthesiologists, Buenos Aires, Argentina, March 25-30, 2012.
- Christine W. Hunter, Shaul Cohen, Sal Zisa, Sana M. Shaikh, Jorge Mendez, Tejal Mehta, Ryan Sison, Anna Pashkova, Sahebjit Bhasin and James Tse: Is High Nasal Cannula Oxygen Flow More Efficient than a No-Cost TSE “Mask” in Reducing Severe Desaturation in Patients under Deep Propofol Sedation during Upper GI Endoscopy? Accepted as Poster Presentation at NYSSA 66th PGA, NY, NY, Dec 14-18, 2012.
- Mohammed Y. Khan, Leigh Nelson-Lane, Shaul Cohen, Sylviana Barsoum, Shruti Shah and James Tse: Does No-Cost TSE “Mask” Improve Oxygenation and Prevent Severe Desaturation in Patients under Propofol Sedation during Short Colonoscopy? Poster Presentation (Abstract 018) at the SAMBA 26th Annual Meeting, San Antonio, TX, May 5-8, 2011.
- Maria Negron-Gonzalez, Shaul Cohen, Tejal Mehta, Sylviana Barsoum, Christine W. Hunter and James Tse: Pre-Oxygenation with No-Cost TSE “Mask” Reduces Severe Desaturation in Obese Patients under Deep Propofol Sedation during Colonoscopy. Poster Presentation (S-07) at the International Anesthesia Research Society 2011 Annual Meeting, Vancouver, British Columbia, Canada, May 21-24, 2011.
- James Tse, Leigh Nelson-Lane, Shruti Shah, May Anne Fernandez and Shaul Cohen: A Simple Technique to Improve Oxygenation and Prevent Severe Desaturation in Patients under Deep Propofol Sedation during Short Colonoscopy. Poster Presentation (A543) at the 2011 ASA Annual Meeting, Chicago, IL, Oct 2011.
- Shruti Shah, Shaul Cohen, May Fernandez, Leigh Nelson-Lane, Sumita Bery, Sana Shaikh, Harris Shaikh and James Tse: No-Cost TSE “Mask” Prevents Severe Desaturation in Patients under Deep Propofol Sedation during Short Colonoscopy. Poster Presentation (P9014) at the NYSSA 65th PostGraduate Assembly in Anesthesiology, NY, Dec 9-13, 2011.
- James Tse, Shaul Cohen, May Fernandez, Kristen Dauphinee, Sylviana Barsoum, Mordechai Bermann, Melissa S. Wu, Jane Kim, Candy Anim and Christine W. Hunter: Is No-Cost TSE “Mask” More Efficient than High Nasal Cannula Oxygen Flow in Reducing Severe Desaturation in Patients under Deep Propofol Sedation during Colonoscopy? Poster Presentation (A345) at the 2012 ASA Annual Meeting, Washington, D.C., Oct 13-17, 2012.
- Shruti Shah, Mordechai Bermann, Candy Anim, Laurie Spina, Adil Mohiuddin and James Tse: TSE “Mask” Improves Oxygenation and Prevents Severe Desaturation in Elderly Patients under Deep Propofol Sedation during Colonoscopy. Poster Presentation (A973) at the 2012 ASA Annual Meeting, Washington, D.C., Oct 13-17 2012.
- Laurie Spina, Shaul Cohen, Sabrina Haque, Christian McDonough, Jorge Mendez, Andrew Burr, Ryan Sison, Christine Park No, Jaimie John and James Tse: Does Pre-Oxygenation with a No-Cost TSE “Mask” Reduce Severe Desaturation in Elderly Patients under Deep Propofol Sedation during Colonoscopy? Accepted as Poster Presentation at NYSSA 66th PGA, NY, NY, Dec 14-18, 2012.
- Shaul Cohen, Christian McDonough, Heather Skiff, Sal Zisa, Sameet Syed, Jane Kim, Sana M. Shaikh, Noah Rolleri, Christine Park No and James Tse: Is High Nasal Cannula Oxygen Flow More Efficient than a No-Cost TSE “Mask” in Reducing Severe Desaturation in Patients under Deep Propofol Sedation during Colonoscopy? Accepted as Poster Presentation at NYSSA 66th PGA, NY, NY, Dec 14-18, 2012.
- John Denny, Jana Janco, Vincent Cirella, Shaul Cohen, Gina George and James Tse: Does No-Cost TSE "Mask" Improve Oxygenation and Reduces Severe Desaturation in Obese Patients during Cardioversion/AICD Testing? Poster Presentation (A545) at the 2011 ASA Annual Meeting, Chicago, IL, Oct 2011.
- Shaul Cohen, Vincent Cirella, Christine W. Hunter, Gina George, Jana Janco, Akwasi Amponsah, A. Sahani Panjwani and James Tse: Pre-Oxygenation with No-Cost TSE “Mask” Reduces Severe Desaturation in Obese Patients during Cardioversion/AICD Testing. Poster Presentation (P9016) at the NYSSA 65th PostGraduate Assembly in Anesthesiology, NY, Dec 9-13, 2011.
- Maria Negron-Gonzalez, Dora Zuker, Shaul Cohen, Jana Janco, Christine W. Hunter and James Tse: A Simple Technique to Reduce Severe Desaturation and the Need for Assisted Bag-Mask Ventilation in Obese Patients during Cardioversion/AICD Testing. Poster Presentation (395) at the 15th WFSA World Congress of Anaesthesiologists, Buenos Aires, Argentina, March 25-30, 2012.
- Shaul Cohen, Sylviana Barsoum and James Tse: Pre-Oxygenation with a No-Cost TSE “Mask” Prevents Severe Desaturation and Reduces the Need for Bag-Mask Ventilation in Propofol-Sedated Elderly Patients during Cardioversion/AICD Testing. Poster Presentation (S285) at the IARS 2012 Annual Meeting, Boston, MA, May 18-21, 2012.
- Julie Mathew; Shaul Cohen; Kristen Dauphinee; Christine W. Hunter and James Tse: Pre-Oxygenation with No-Cost TSE “Mask” Prevents Severe Oxygen De-Saturation in Elderly Patients under Deep Propofol Sedation during Retrobulbar Block. Abstract 020 at the Society of Ambulatory Anesthesia 26th Annual Meeting, San Antonio, TX, May 5-8, 2011.
- James Tse, Sylviana Barsoum, Kristen Dauphinee, Candy Anim, Dora Zuker, Tejal Mehta, Julie Mathew, Melissa S. Wu and Shaul Cohen: Does Pre-Oxygenation with No-Cost TSE “Mask” Reduce Severe Desaturation in Elderly Patients under Deep Propofol Sedation during Retrobulbar Block? Poster Presentation (P9017) at the NYSSA 65th PostGraduate Assembly in Anesthesiology, NY, Dec 9-13, 2011.
- James Tse, Dora Zuker, Maria Negron-Gonzalez, Kristen Dauphinee, Sylviana Barsoum and Shaul Cohen: Pre-Oxygenation with No-Cost TSE “Mask” Reduces Severe Desaturation in Elderly Patients under Deep Propofol Sedation during Retrobulbar Block. Poster Presentation (62) at the 15th WFSA World Congress of Anaesthesiologists, Buenos Aires, Argentina, March 25-30, 2012.
- Jana Janco, Shaul Cohen, Christine W. Hunter, Sylviana Barsoum, John Denny, Scott Mellender, Christian McDonough, Julian Kertsman, Mohammed Y. Khan and James Tse: A Simple Technique to Improve Oxygenation and Reduce the Risk of Fire Hazard in Obese Patients under MAC/TIVA. Poster Presentation at the 2011 NJSSA.
- Mohammed Y. Khan, Shaul Cohen, Christine W. Hunter, Caroline Zawilski and James Tse: Does No-Cost TSE “Mask” Improve Oxygenation and Reduce the Risk of Fire Hazard in Propofol-Sedated Patients during Short Surgical Procedures? Poster Presentation (Abstract 014) at the Society of Ambulatory Anesthesia 26th Annual Meeting, San Antonio, TX, May 5-8, 2011.
- Michael Wong, Christine W. Hunter, Shaul Cohen, Branson Collins and James Tse: A Simple Technique to Improve Oxygenation and Reduce the Risk of Fire Hazard in Propofol-Sedated Patients during Short Surgical Procedures. Poster Presentation (A544) at the 2011 ASA Annual Meeting, Chicago, IL, Oct 2011.
- Christine W. Hunter, Shaul Cohen, Branson Collins, Tejal Mehta, Michael J. Wong, Mohammed Y. Khan, Oliver Choo, Gianna Casini and James Tse: No-Cost TSE “Mask” Reduce Severe Desaturation and the Risk of Fire Hazard in Propofol-Sedated Patients during Short Surgical Procedures. Poster Presentation (P9015) at the NYSSA 65th PostGraduate Assembly in Anesthesiology, NY, Dec 9-13, 2011.
- James Tse, Maria Negron-Gonzalez, Dora Zuker, Christine W. Hunter, Michael J. Wong and Shaul Cohen: A Simple Technique to Prevent Severe Desaturation and Reduce the Risk of Fire Hazard in Propofol-Sedated Patients during Short Surgical Procedures. Poster Presentation (393) at the 15th WFSA World Congress of Anaesthesiologists, Buenos Aires, Argentina, March 25-30, 2012.
- Denny, Pantin: TEE Evaluation of Aortic Atherosclerosis in Elderly Patients Scheduled for CABG, ASA, Washington, DC, 2012.
- Ginsberg, Denny, Pantin, Mohiuddin, Waskey: Use of a Bracket to Simplify Invasive Pressure Monitoring, ASA, Washington, DC, 2012.
- Stein MH: Anesthesia guidelines for the obese patient. Society of Bariatric Anaesthetists, London, UK, September 2011.
- Stein MH, Nightingale C, Redman J, Kennedy NJ. Anaesthesia for the obese patient- the Society of Bariatric Anaesthetists’ guidelines. Society of Bariatric Anaesthetists, London, UK, September 2011.
- Stein MH: Anesthesia guidelines for the obese patient. Society of Anesthesia and Sleep Medicine, Chicago, IL, October 2011.
- Stein MH, Nightingale C, Redman J, Kennedy NJ. Anaesthesia for the obese patient- the Society of Bariatric Anaesthetists’ guidelines. Society of Anesthesia and Sleep Medicine ,Chicago, IL, October 2011.
- Gina George, Sameet Syed M.D., Shaul Cohen, M.D., Shruti Shah M.D., Christine Park No B.A., M.S, Anna Pashkova B.A., Arpan Patel B.S., Noah Rolleri B.S., Christine W. Hunter M.D., CSE for Cesarean Section: Gertie Marx versus PENCAN Spinal Needles. Poster Presentation: ASRA 2012, Miami, FL, November 2012. (Accepted)
- Christine Park No B.A., M.S, Shaul Cohen, M.D., Shruti Shah M.D., Sameet Syed M.D., Anna Pashkova B.A., Arpan Patel B.S., Noah Rolleri B.S., High Spinal Anesthesia during Epidural-PCA for Post-Cesarean Analgesia. Poster Presentation: ASRA 2012, Miami, FL, November 2012. (Accepted)
- Amponsah A, Cohen S, Kiel S, Hall D, LaSalle S, Sakr A, Sakr E: Does the addition of ondansetron to IV-patient controlled naloxone further improve post C/S epidural-fentanyl-induced pruritus treatment? Poster Presentation: The Annual Meeting of the American Society of Regional Anesthesia & Pain Medicine. 2011
- Amponsah A, Cohen S, Kiel S, LaSalle S, Shah S, Ginsberg S, Daley W, Hunter CW: Can Hypotension from intrathecal Ropivacaine for C/S be prevented with 6% Hetastarch more than Prophylactic IV Ephedrine? Poster Presentation: The 36th Annual Regional Anesthesia Meeting and Workshops, Las Vegas, Nevada, May 2011.
- Kim J, Cohen S, Davidov T, Hunter WC: Asymptomatic thyromegaly as a cause of high intraoperative peak inspiratory airway pressure NYSSA, MCC-7028, 2011 Poster Presentation: 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Shaikh H, Shaikh S, Cohen S, Morgan S, Hunter CW: Allergic Reaction to r-ATG (Thymoglobulin, rabbit Anti-thymocyte Globulin) during Kidney Transplant. NYSSA, MCC-7082, 2011.
- Kaufman M, Cohen S, Hochkeppel J, Casini G: Excessive CSF loss via Epidural Needle from Spinal needle Dural Puncture During CSE for Cesarean Section NYSSA, MCC 7020, 2011 Poster Presentation: 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Cohen S, Casini G, Hochkeppel J, Estrada C: Unexplained Loss of Consciousness by Patient with Abruptio Placentae: NYSSA, MCC 7021, 2011Poster Presentation: 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Cohen S, Shruti S, Jian W, Barsoum S, Hochkeppel J, Estrada C, Janco J, Berman S: Arrow versus B. Braun Springwound Closed Tip Epidural Catheter for Epidural block in Obstetric Patients. NYSSA, P-9068, 2011 Poster Presentation: The 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Barsoum S, Cohen S, Shruti S, Jian W, Hochkeppel J, Estrada C, Janco J, Berman S: Can Electrical Median Nerve Stimulation further reduce the incidence of Nausea and Vomiting (N/V) during Cesarean Section (C/S) with Combined Spinal Epidural (CSE) treated with Ondansetron and Metoclopramide. NYSSA, P-9069, 2011 Poster Presentation: The 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Spence N, Kalyam K, Cohen S, Shah S, Nelson-Lane L, Shkolnikova T, Kim J, Fernandez MA, Tse J, Hunter CW: Does the addition of intravenous lidocaine to propofol blunt the response to noxious stimuli upon insertion of endoscope for upper endoscopy? Poster Presentation: : Research Poster Session, UMDNJ-RWJ Medical School, New Brunswick, NJ, November 2011.
- Kalyam K, Spence N, Cohen S, Shah S, Janco J, Fernandez MA, Patel P, Hunter CW: Epidural-PCA Analgesia for Labor pain: Private versus Staff Patients.?Poster Presentation: : Research Poster Session, UMDNJ-RWJ Medical School, New Brunswick, NJ, November 2011.
- Shah S, Cohen S, Shaikh S, Shaikh H, Casini G, Hochkeppel J, Wu M: Does Increasing Concentration of Epidural-PCA Fentanyl for Labor Improve Analgesia Without effects on Neonate? NYSSA, P-9043:2011 Poster Presentation: The 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Shah S, Cohen S, Hochkeppel J, Janco J, Fernandez MA, Casini G, Nelson-Lane L, Patel P: Epidural-Fentanyl-Induced Pruritis: Self-Administered versus Nurse-Administered IV Naloxone. NYSSA, P-9044:2011 Poster Presentation: : The 65th Annual meeting of NY Society of Anesthesiologist NY, NY December 2011.
- Shah S, Cohen S, Zisa S, Adil Mohammed, Collins B, Patel P, Barsoum S, : Does the addition of ondansetron to IV-Patient controlled analgesia with naloxone further improves Post C/S Epidural –fentanyl-induced pruritus: S-333 IARS 2012. Poster Presentation:International Anesthesia Research Society, Boston, MA 2012.
- Patel P, Cohen S, Shah S, Rao M, Fernandez M, Chhokra R, Barsoum S, Tse J, Hunter CW : A comparison between combined spinal-epidural anesthesia (cse) with or without epidural saline administration for cesarean section. Abstract # 66, 2012. Poster Presentation: 37th Annual Regional Anesthesia Meeting and Workshops March 15-18, 2012, Hilton San Diego Bayfront, San Diego, California.
- Patel P, Cohen S, Shah S , Rao M , Fenandez M, Chhokra R, Barsoum S, Tse J, Hunter CW Does the addition of phenylephrine to IV ephedrine for prophylactic IV ephedrine further reduces the incidence of hypotension from intrathecal ropivacaine for C/S? Abstract # 47 2012 Poster Presentation: 37th Annual Regional Anesthesia Meeting and Workshops March 15-18, 2012, Hilton San Diego Bayfront, San Diego, California.
- Fernandez M, Cohen S, Mohiuddin A, Shah S, Patel P, Patel A, Mehta T. Can suturing the epidural catheter further reduce the incidence of failed epidural blocks in obstetric patients? Poster Presentation: NJSSA April 21 2012. New Jersey.
- Janco J, MD, Cohen S, MD, Mohiuddin A, MD, Shah S, MD, Patel P, MD, Mehta T, MD, Sameet S, MD. Does the addition of intravenous lidocaine to propofol blunt the response to noxious stimuli upon insertion of endoscope for upper endoscopy? Poster Presentation: NJSSA April 2012, New Jersey.
- George G, Cohen S, Tse J, Mohiuddin A, Patel A: Does the addition of intravenous lidocaine to propofol blunt the response to noxious stimuli upon insertion of endoscope for upper endoscopy? Poster Presentation: Samba Miami Beach, Florida, May 2012.
- Mohiuddin A, Patel A, Cohen S, Chhokra R, Hunter C: A complete left bronchus occlusion by mucous plug mimicking tension pneumothorax. Poster Presentation: Samba, Miami Beach, Florida, May 2012.
- Mohiuddin A, Cohen S, Shah S, Patel A, Hunter C: Cardiac arrest upon induction of IV sedation to hemodialyzed patient for colonoscopy. Poster Presentation: Samba, Miami Beach, Florida, May 2012.
- Sakr A, Cohen S, Mohiuddin A, Shah S, Mellender S, Patel P, Hunter C.W : Can we offer Spheno-palatine ganglion block for our obstetric patients following accidental dural puncture? Poster Presentation : ASA Annual Meeting, October 13-17, 2012, Washington, DC. (Accepted)
- Shah S, Cohen S, Mohiuddin A, Denenberg H, Chhokra R, Barsoum S, Hunter C W: Should we offer epidural PCA analgesia with ambulation for multiparae for Labour pain? Poster Presentation: ASA Annual Meeting, October 13-17, 2012, Washington, DC.
- Ginsberg S H, Solina, R A Syed S, Cohen S, Zisa S, Hylton A : Equipment availability and patient safety study. Poster Presentation: ASA Annual Meeting, October 13-17, 2012, Washington, DC.
- Shah S, Shkolnikova T, Anim C, Cohen S, Mohiuddin A, Hunter C W : Evaluation of operating room (OR) delays at RWJMS. Poster Presentation: ASA Annual Meeting, October 13-17, 2012, Washington, DC.
- Oren Y. Ambalu, Shaul Cohen, Arpan G. Patel, Tatyana Shkolnikova and Jaimie John: Labor Epidural for a Parturient With a History of Myelomeningocele. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Arpan G Patel, Shaul Cohen, Oren Y Ambalu, Shruti Shah, Achillina Rianto, Jamie John, Renu Chhokra and Christine W Hunter: Epidural-PCA Analgesia for Primiparae with Labor Pain: Labor and Delivery Outcome 2010-2011 versus 1998-1999. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Mohammad A Chaudhry, MD*, Shaul Cohen, MD, Shruti Shah, MD, Anna A Pashkova, BA, Arpan Patel, BS, Noah Rolleri, BS and Christine Park No: Management of Rare Coagulation Defect in a Parturient Undergoing Cesarean Delivery. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Harris Shaikh, Shruti Shah, Shaul Cohen, Aliraza Dinani, Noah Rolleri, Anna A Pashkova, Christine Park No, Sylviana Barsoum and Christine W Hunter, MD: Successful Treatment of Acute Allergic Reaction to Tranexamic Acid During Total Knee Arthroplasty. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Renu Chhokra, Adil Mohiuddin, Shaul Cohen, Shubhankar Chhokra, Oren Y Ambalu, Sahebjit Bhasin and Arpan G Patel: Does the application of ice at the IV site further reduce burning sensation from IV lidocaine and propofol induction for endoscopy? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Renu Chhokra, Adil Mohiuddin, Shaul Cohen, Shubhankar Chhokra, Shrutie Shah, Oren Y Ambalu, and May A Fernandez: Can ice application at the IV site be used as an alternative for IV lidocaine upon propofol injection in endoscopy patients? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York. (Submitted)
- Renu Chhokra, Adil Mohiuddin, Shaul Cohen, Shubhankar Chhokra, Shrutie Shah, Oren Y Ambalu, and May A Fernandez: Can ice application at the IV site be used as an alternative for IV lidocaine upon propofol injection in endoscopy patients Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Sal Zisa, Adil Mohiuddin, Shaul Cohen, Arpan G Patel, Oren Y Ambalu, Shruti Shah and Christine W Hunter: Does the administration of mixture of lidocaine with propofol for IV induction attenuate the burning sensation more than separately injecting lidocaine prior to propofol?Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Gina George, Shaul Cohen, Oren Y Ambalu, Arpan G Patel, Anna Pashkova and Christine H Hunter: Acute Postoperative Negative Pressure Pulmonary Edema Immediately Following Extubation. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Shaul Cohen, Mordechai Bermann, Alann Solina, Kristen Dauphinee, May A Fernandez, Oren Y Ambalu, Arpan G Patel and Jane Kim: Unrecognized Fatal Meningitis in the Postpartum Period Following an Uneventful Labor and Delivery with Epidural Analgesia. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Tatyana Shkolnikova, Shaul Cohen, Adil Mohiuddin, Sylviana Barsaum, Shruti Shah, Oren Y Ambalu, Anna Pashkova and Renu Chhokra: Does Reduced Concentration of Epidural-PCA Ropivacaine for Labor Pain with Maternal Ambulation Improve Labor and Delivery Outcome? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Shruti Shah, Melissa Wu, Shaul Cohen, Adil Mohiuddin, Oren Y Ambalu, Arpan G Patel, Ashraf Sakr and Renu Chhokra: Does stylet reinsertion upon piercing the ligamentum flavum with an epidural needle reduce the incidence of accidental dural puncture? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Jane Kim, Shaul Cohen, Oren Y Ambalu, Arpan G Patel, Shruti Shah, Jaimie John and James Tse: Does the addition of intravenous lidocaine to propofol blunt the response to noxious stimuli upon insertion of endoscope for upper endoscopy Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- May A Fernandez, Shaul Cohen, Adil Mohiuddin, Shruti Shah, Oren Y Ambalu, Arpan G Patel, Sahebjit Bhasin and Tejal Mehta: Suturing the Epidural Catheter Reduces the Incidence of Failed Epidural Block in Obstetric Patient. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Harris Shaikh, Shaul Cohen, Adil Mohiuddin, Tejal Mehta, Oren Y Ambalu, Arpan G Patel, Jaimie John and Sylviana Barsoum: Epidural-PCA For Labor Pain: Do Multiparae Require Less Epidural Medications Than Primiparae? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Shaul Cohen, Ashraf Sakr, Adil Mohiuddin, Shruti Shah, Arpan G. Patel, Anna Pashkova, Vishal Patel and Christine W. Hunter: Can Spheno-palatine ganglion block be used routinely for our obstetric patients following accidental dural puncture for PDPH treatment? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Ankit Kapadia, Shaul Cohen, Adil Mohiuddin, Arpan G. Patel, Anna Pashkova, Vishal Patel, Noah Rolleri and Christine W. Hunter: Combined Spinal Epidural Anesthesia for Cesarean Section: Gertie Marx versus PENCAN Spinal Needles. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Noah Rolleri, Shaul Cohen, Mary Corless, Anna Pashkova, Sameet Syed, Oren Y Ambalu, Vishal Patel, and Christine W Hunter: Severe Bradycardia Following Cardioversion for Atrial Fibrillation. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Anna Pashkova, Shaul Cohen, Arpan G. Patel, Noah Rolleri, Sameet Syed, Sahani Panjwani, Sylviana Barsoum, Kristen Dauphinee and Christine W. Hunter: High Spinal Anesthesia during Epidural-PCA for Post-Cesarean Analgesia. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Sal Zisa, Shaul Cohen, Sameet Syed, Shruti Shah , Anna Pashkova, Arpan G Patel, Noah Rolleri and Christine W Hunter: Anesthetic Management of Parturient with Cardiomyopathy Scheduled for Urgent Cesarean Section. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Christine Park No, Shaul Cohen, Sameet Syed, Arpan G Patel, Anna Pashkova, Noah Rolleri, Shruti Shah, Sana Shaikh and Christine W Hunter: Can Electrical Median Nerve Stimulation Replace Ondansetron and Metoclopramide For Routine Use To Reduce the Incidence of Nausea and Vomiting (N/V) during Cesarean Section (C/S) with Combined Spinal Epidural (CSE)? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Sameet Syed, Gina George, Shaul Cohen, Arpan G Patel, Anna Pashkova, Noah Rolleri, Adil Mohiuddin and Christine W Hunter: Dog Bite Throat Trauma Causing Distortion of Airway Anatomy, Misplacement of Endotracheal Tube, and Emergency Tracheostomy? Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Heather Skiff, Shaul Cohen, Anna A Pashkova, Noah Rolleri, Arpan Patel, Shruti Shah, Sameet Syed and Christine W Hunter: Central Anticholinergic Syndrome: A Forgotten Diagnosis. Poster Presentation: NYSSA 66th PGA, December 15-17, 2012, New York.
- Oliver Choo, Christine Park No, Shaul Cohen M.D., M.D., Shruti Shah M.D., Sameet Syed M.D., Anna Pashkova B.A., Arpan G. Patel B.S., Noah Rolleri B.S., May Anne Fernandez M.D., Does the addition of phenylephrine to prophylactic IV ephedrine further reduce the incidence of hypotension from intrathecal ropivacaine for C/S? Poster Presentation: ASRA 2012, Miami, FL, November 2012.
- Sloane Yeh, Sameet Syed M.D., Shaul Cohen, M.D., Shruti Shah M.D., Christine Park No B.A., M.S, Anna Pashkova B.A., Arpan Patel B.S., Noah Rolleri B.S., Christine W. Hunter M.D., Epidural-Fentanyl-Induced Puritis: Self-Administered Versus Nurse-Administered Intravenous Naloxone. Poster Presentation: ASRA 2012, Miami, FL, November 2012.
- Mike Wong, Sameet Syed M.D., Shruti Shah, M.D., Shaul Cohen M.D., Christine Park No B.A., M.S, Anna Pashkova B.A., Noah Rolleri B.S., Arpan Patel B.S., Tatyana Shkonikova M.D., Does suturing the epidural catheter reduces the incidence of failed epidural block in obstetric patient. Poster Presentation: ASRA 2012, Miami, FL, November 2012.
Full Listing of Clinical Services
The New Jersey Pain Institute
The Department of Anesthesiology and Perioperative Medicine operates a comprehensive multidisciplinary pain management center. The New Jersey Pain Institute offers diagnosis and treatment for acute, chronic and cancer pain problems. We work with the Oncology Divisions at Robert Wood Johnson Medical School and Cancer Institute of New Jersey (CINJ) to provide the most up-to-date pain management techniques for cancer pain patients, including implanted epidural catheters and neuroablative blocks under fluoroscopic and CT scan guidance.
The Chronic Pain Management Service
Evaluates and treats a diversity of pain problems such as:
- Discogenic and axial low back pain
- Discogenic and axial neck pain
- Neuropathic pain, myofascial pain
- Post cervical laminectomy pain
- Post lumbar laminectomy pain
- Headaches
Nerve Blocks
We perform nerve blocks including:
- cervical, thoracic and lumbar epidural blocks
- brachial plexus blocks
- lumbar-sacral plexus blocks
- stellate ganglion blocks
- lumbar sympathetic blocks
- facet joint blocks
- nerve root injections and cranial nerve blocks under fluoroscopic guidance
- other peripheral nerve blocks
State of the Art Pain Treatments
We also perform state of the art pain treatments such as:
- cryoanalgesia
- radiofrequency neurolysis
- spinal cord stimulators
- percutaneous disc compression
- kyphoplasty
- minimally invasive lumbar decompression (MILD procedure)
- endoscopic rhizotomy
- discography
- nucleoplasty and intrathecal pump placements
Information for Parents
Being Prepared
Pain is an uncomfortable feeling that tells you something may be wrong in your body. When there is an injury to your body, such as through surgery, nerve cells send signals into the spinal cord and then up to the brain. Pain medicine blocks those signals or reduces their effect on the brain. After your child's surgery or treatment, your nurses and doctors will ask you and your child about the pain because they want your child to be comfortable. Both medicine and non-medicine treatments can help to prevent and control pain.
-
- Will there be much pain after the surgery or treatment?
- Where will the pain be?
- How long is the pain likely to last?
-
- How will pain be controlled after surgery or treatment?
- Tell the doctor or nurse what has worked for your child in the past and what has not worked in the past.
- Ask about possible side effects that may occur with pain medicine.
- Tell the doctor or nurse about your concerns
- Ask your nurse about non-medicine options to decrease your child's pain. These include rocking and holding your child; hot or cold packs; music, stories, or videos to distract your child; and techniques to help your child relax.
-
They may ask your child to rate the pain on a scale of 0 to 10, with 0 being no pain and 10 being the worst pain they can imagine, or to choose a face from the Faces Scale that best describes the pain. Your child may also choose to draw his or her own rating scale to describe pain. You may need to help your child with these ratings:
- It may be helpful to have your child set a pain control goal, such as having no pain greater than a "2" on the scale.
- For children who are not able to use the pain scales, the doctors and nurses will rely on other signals of pain, such as increased heart rate, crying or grimacing, and on your judgment of your child's level of pain to guide their pain relief efforts.
- Tell your doctor or nurse about any pain that won't go away.
- Stick with the pain control plan if it is working. If it isn't working, your doctors and nurses can change the plan.
-
- Something should be done about the pain as soon as it starts. It is more difficult to ease pain once it has become established. This is a key step in proper pain control.
- The nurses may ask your child to accept pain medicine at set times for the first 24 hours after surgery. Our goal is to prevent or minimize pain.
- Pain medication can be given by mouth, into the bloodstream (intravenous or IV) or into the rectum (suppository) or through a catheter placed painlessly into the spinal area (epidural).
- If you know your child's pain will get worse when he or she starts walking or doing breathing treatments, ask for pain medicine first.
Copyright protected material used with permission of the authors and the University of Iowa’s Virtual Hospital.
